School-Based Smartphone Interventions Effective Obesity Prevention for Boys
Researchers of a study in Pediatrics studied the effectiveness of a school-based intervention using mobile apps in changing teens’ body weight, eating and activity behaviors, and screen-time. The researchers focus on boys in low-income areas (assuming they are the highest risk group), and conclude that school-based smartphone interventions can be successful in reducing the consumption of sugared drinks and increasing physical fitness. Positive changes in physical activity and physical appearance (BMI, waist size, body fat) seem harder to accomplish. The researchers give additional advice for future smartphone app features, since they experienced difficulties with creating engagement around the app and its accompanying physical activity tracking system.
Take aways
- Previous research shows that standalone health apps can improve girls’ fruit and vegetable intake and reduce their sugared beverages consumption (especially when these apps contain motivators to do so).
- This study shows that school-based interventions using mobile apps can also reduce boys’ consumption of sugary drinks and improve their physical fitness.
- Increases in screen-time can be limited by the app as well.
- Even when mobile apps are developed to strengthen school-based programs, app developers need to think about the implemented features to support ongoing engagement among teens. Motivations to wear required hardware (e.g., pedometers to count steps) must be clear and given as well, since usage of these wearables is not always popular.
Study information
The question?
Can school-based interventions using mobile apps positively change boys’ body weight, eating and activity behaviors, and screen-time?Who?
361 12- to 14 year old boys attending schools in low-income areas (mean age: 12 years old)Where?
AustraliaHow?
The boys were divided in two groups. In the intervention group, they followed the 20-week intervention program “ATLAS”, a school-based smartphone intervention to prevent unhealthy weight gain. In the control group, no intervention was followed, the boys only participated in usual school sports and physical education lessons.
Prior to the intervention, boys’ height, weight, waist size, and body fat were obtained. Their sugared beverages consumption, screen-time, physical activity (through pedometers that counted steps), physical fitness (push-up repetitions, grip strength), and resistance training skills (through six different strength exercises) were obtained as well (for both groups before and 8 months after the start of the intervention).
During the intervention, boys in the intervention group received physical activity sessions (sometimes during lunch-time), and informational interactive seminars about for instance screen-time, and physical activity consequences. Additionally, they were provided with a pedometer to monitor and track activities, and to set goals via the app. So-called “push notifications” were also sent with motivating and informative messages.
Facts and findings
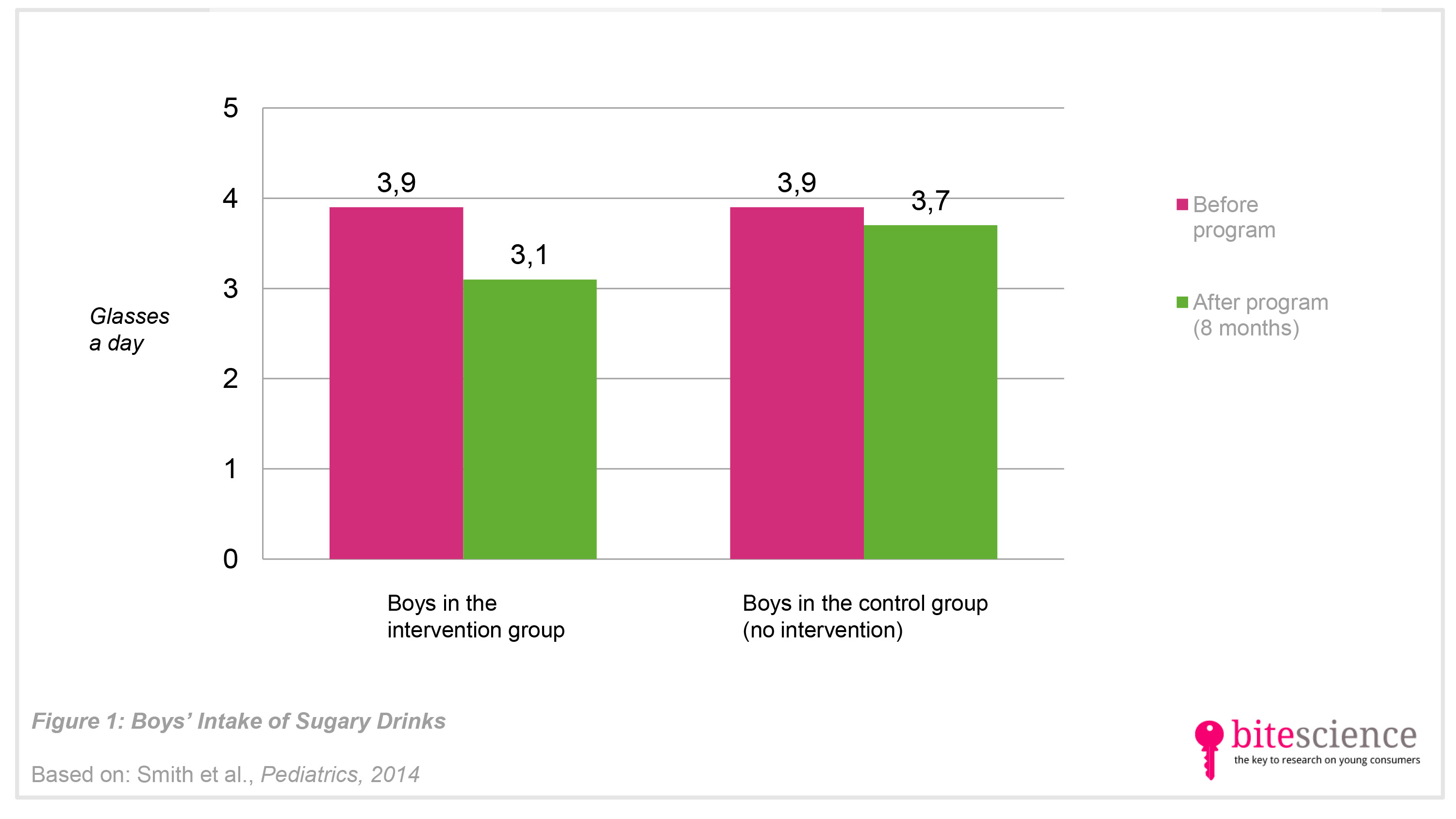
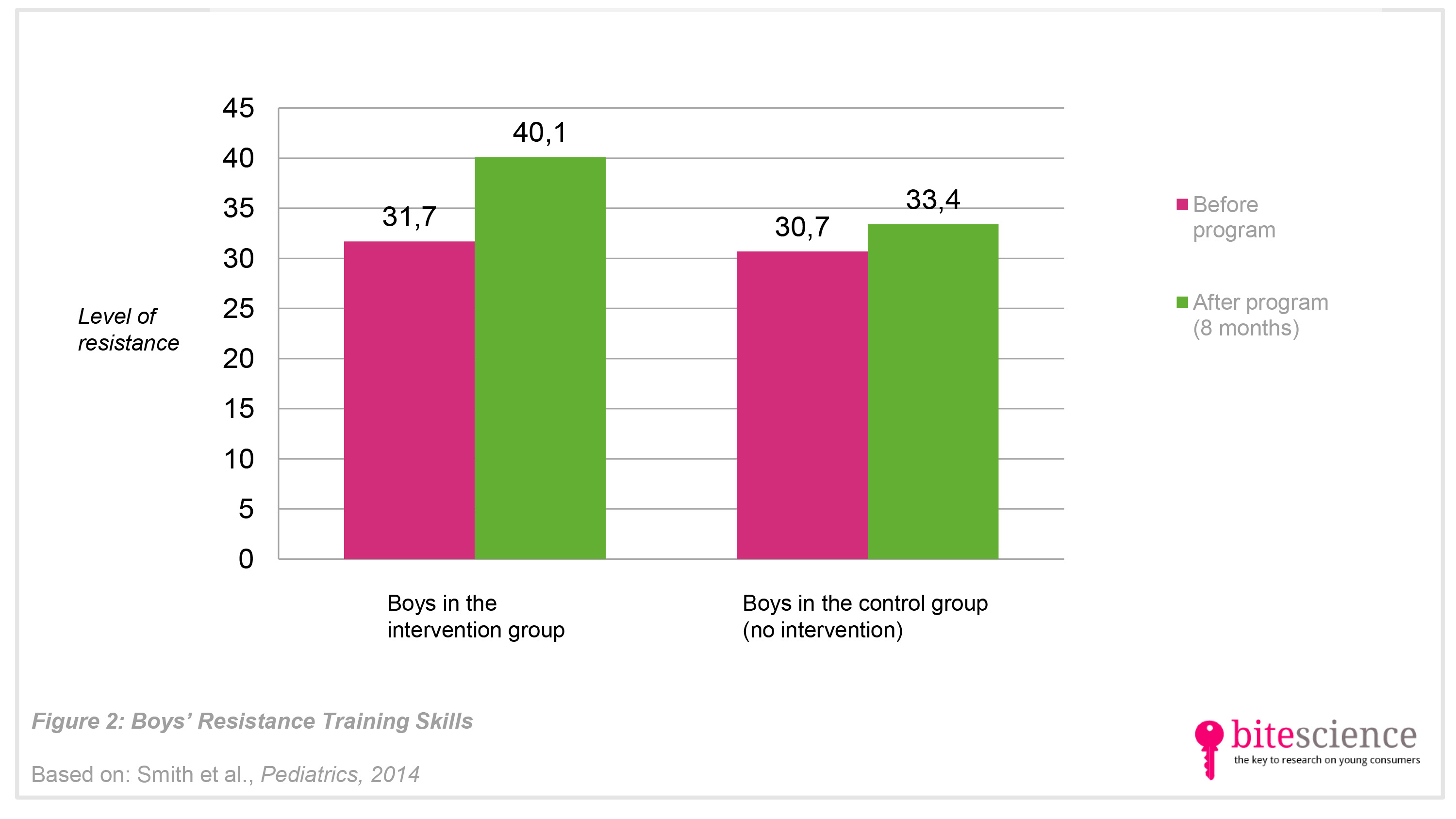
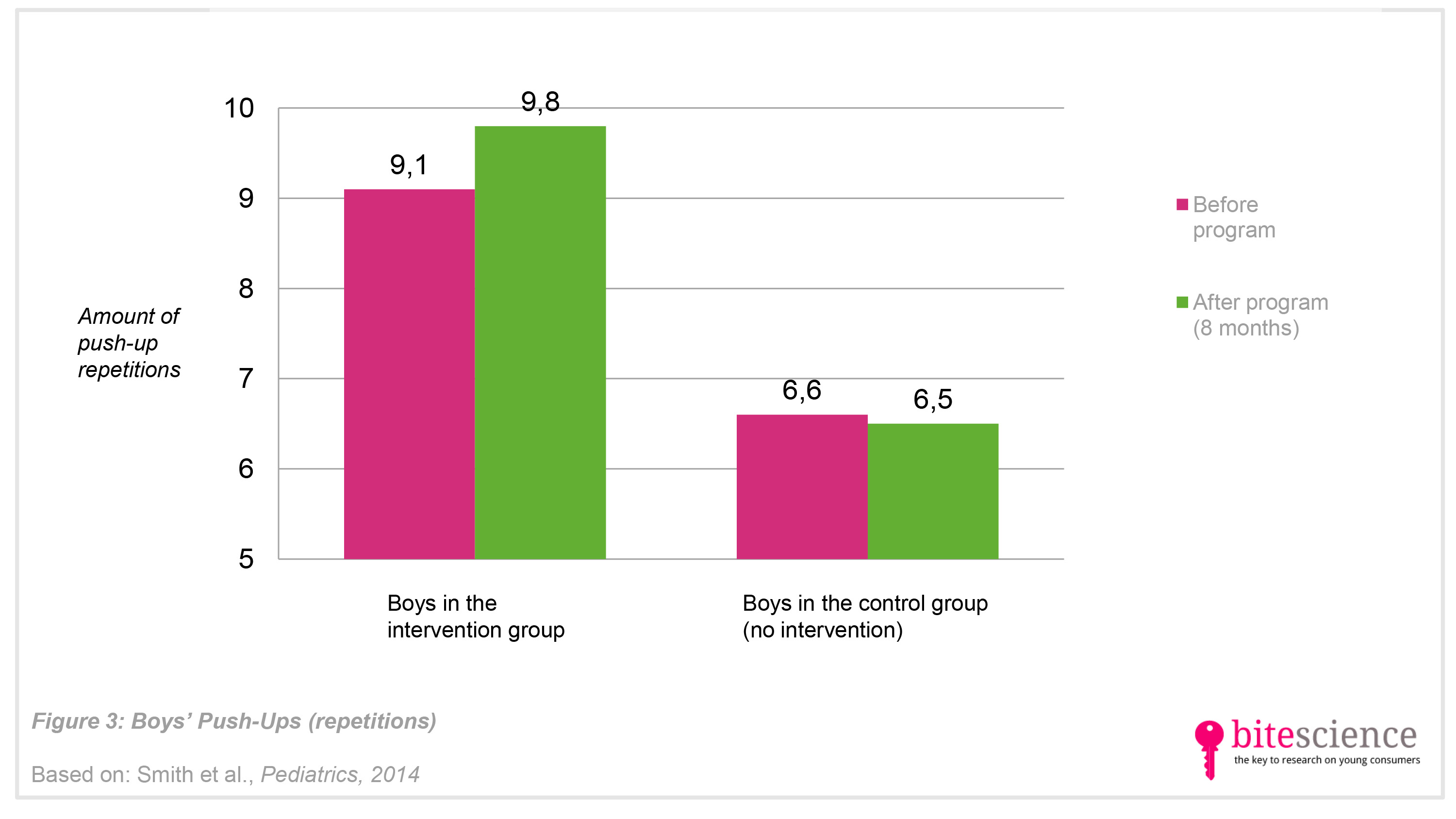
- In the group who participated in the 20-week school-based intervention, the boys reduced their consumption of sugared beverages and improved their physical fitness (resistance training skills, and muscular fitness) more after the program than those who did not follow the intervention (see Figure 1, 2 & 3).
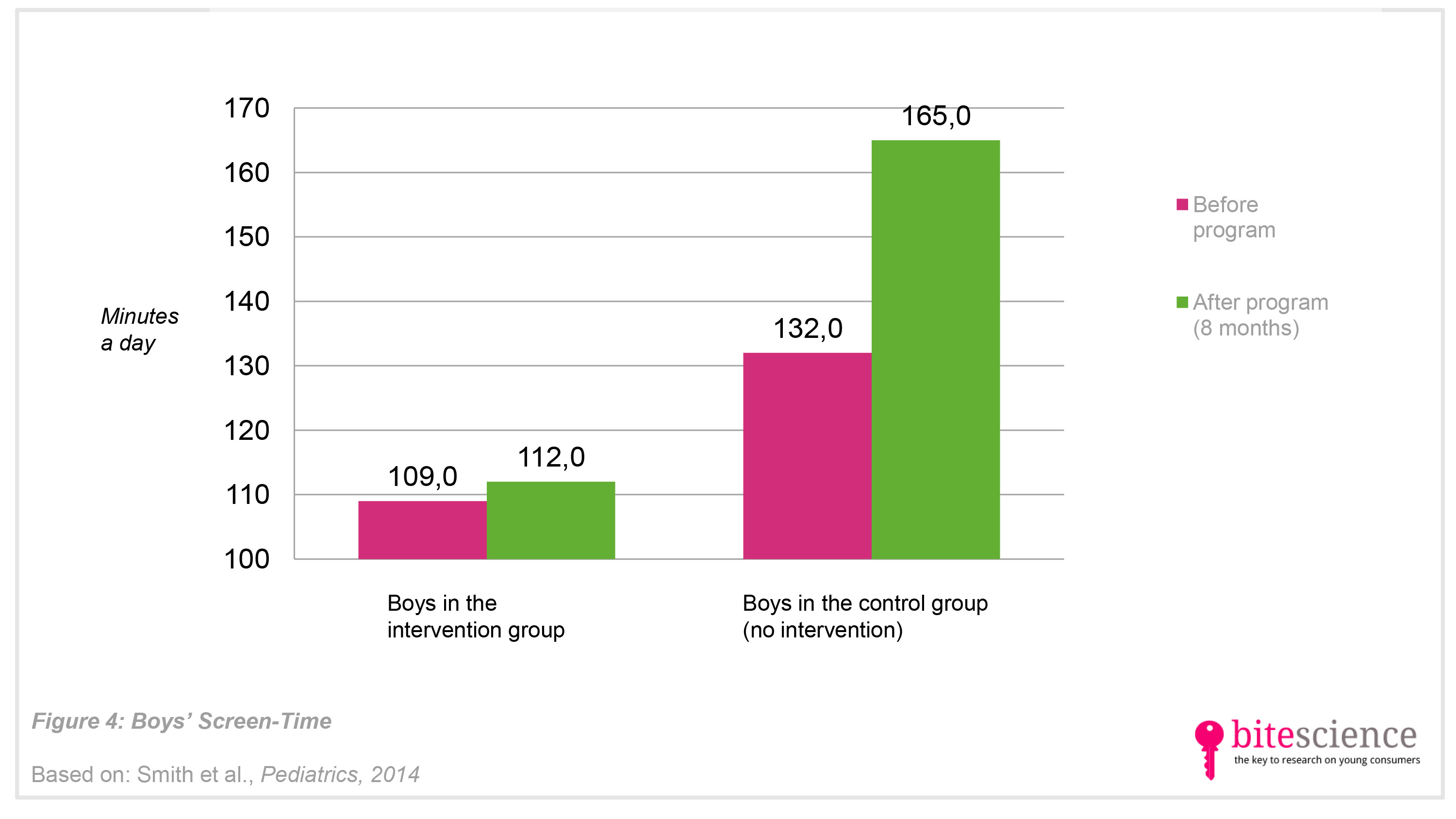
- Despite the fact that the boys in the intervention group unexpectedly increased their screen-time after the intervention with 3 minutes, there was a significant difference with those in the control group who reported an increase of 33 minutes after 8 months (see Figure 4).
- It remains unclear why there was an increase in screen-time overall, but the results imply that screen-time increases were minimized because of the intervention.
- The school-based intervention did not have an impact on boys’ BMI, waist size, percentage of body fat or physical activity (i.e., step counts).
- Results from app and wearable usage showed that:
- less than half of the boys (44%) from the intervention group found the ATLAS app enjoyable to use;
- less than half of the boys from the intervention group, agreed that the reminders through push notifications triggered them to be more active, reduce their screen time, and drink fewer sugary drinks;
- only 30% used their pedometer often, and 44% said they used it sometimes.
- Since boys did not use the app that much for self-monitoring and goal setting, the researchers advised that future smartphone apps should integrate more stimulating features (e.g., social media linkage, game-elements) to support ongoing engagement.
- Critical note: all of the respondents in this study were boys, so the results might not be representative for all teens.